Topical anesthetics: These medicines can cause seizures or a condition called methemoglobinemia which keeps the blood from carrying oxygen to the tissues. Be especially careful with teething gels, hemorrhoid preparations, anti-itch creams, and sunburn relief agents.Poisoning
Acute poisoning is exposure to a poison on one occasion or during a short period of time. Symptoms develop in close relation to the exposure. Absorption of a poison is necessary for systemic poisoning. In contrast, substances that destroy tissue but do not absorb, such as lye, are classified as corrosives rather than poisons. Furthermore, many common household medications are not labeled with skull and crossbones, although they can cause severe illness or even death. In the medical sense, poisoning can be caused by less dangerous substances than those legally classified as a poison.
Chronic poisoning is long-term repeated or continuous exposure to a poison where symptoms do not occur immediately or after each exposure. The patient gradually becomes ill, or becomes ill after a long latent period. Chronic poisoning most commonly occurs following exposure to poisons that bioaccumulate, or are biomagnified, such as mercury, gadolinium, and lead.
Contact or absorption of poisons can cause rapid death or impairment. Agents that act on the nervous system can paralyze in seconds or less, and include both biologically derived neurotoxins and so-called nerve gases, which may be synthesized for warfare or industry.
Inhaled or ingested cyanide, used as a method of execution in gas chambers, almost instantly starves the body of energy by inhibiting the enzymes in mitochondria that make ATP. Intravenous injection of an unnaturally high concentration of potassium chloride, such as in the execution of prisoners in parts of the United States, quickly stops the heart by eliminating the cell potential necessary for muscle contraction.
Most biocides, including pesticides, are created to act as poisons to target organisms, although acute or less observable chronic poisoning can also occur in non-target organisms (secondary poisoning), including the humans who apply the biocides and other beneficial organisms. For example, the herbicide 2,4-D imitates the action of a plant hormone, which makes its lethal toxicity specific to plants. Indeed, 2,4-D is not a poison, but classified as "harmful" (EU).
Many substances regarded as poisons are toxic only indirectly, by toxication. An example is "wood alcohol" or methanol, which is not poisonous itself, but is chemically converted to toxic formaldehydeand formic acid in the liver. Many drug molecules are made toxic in the liver, and the genetic variability of certain liver enzymes makes the toxicity of many compounds differ between individuals.
Toxicology is the study of the symptoms, mechanisms, treatment and diagnosis of biological poisoning.
Exposure to radioactive substances can produce radiation poisoning, an unrelated phenomenon.
Management
- Initial management for all poisonings includes ensuring adequate cardiopulmonary function and providing treatment for any symptoms such as seizures, shock, and pain.
- Injected poisons (e.g., from the sting of animals) can be treated by binding the affected body part with a pressure bandage and placing the affected body part in hot water (with a temperature of 50 °C). The pressure bandage prevents the poison being pumped throughout the body, and the hot water breaks it down. This treatment, however, only works with poisons composed of protein-molecules.[7]
- In the majority of poisonings the mainstay of management is providing supportive care for the patient, i.e., treating the symptoms rather than the poison.
Decontamination
- Treatment of a recently ingested poison may involve gastric decontamination to decrease absorption. Gastric decontamination can involve activated charcoal, gastric lavage, whole bowel irrigation, ornasogastric aspiration. Routine use of emetics (syrup of Ipecac), cathartics or laxatives are no longer recommended.
- Activated charcoal is the treatment of choice to prevent poison absorption. It is usually administered when the patient is in the emergency room or by a trained emergency healthcare provider such as a Paramedic or EMT. However, charcoal is ineffective against metals such as sodium, potassium, and lithium, and alcohols and glycols; it is also not recommended for ingestion of corrosive chemicals such as acids and alkalis.[8]
- Cathartics were postulated to decrease absorption by increasing the expulsion of the poison from the gastrointestinal tract. There are two types of cathartics used in poisoned patients; saline cathartics (sodium sulfate, magnesium citrate, magnesium sulfate) and saccharide cathartics (sorbitol). They do not appear to improve patient outcome and are no longer recommended.[9]
- Emesis (i.e. induced by ipecac) is no longer recommended in poisoning situations, because vomiting is ineffective at removing poisons.[10]
- Gastric lavage, commonly known as a stomach pump, is the insertion of a tube into the stomach, followed by administration of water or saline down the tube. The liquid is then removed along with the contents of the stomach. Lavage has been used for many years as a common treatment for poisoned patients. However, a recent review of the procedure in poisonings suggests no benefit.[11]It is still sometimes used if it can be performed within 1 hour of ingestion and the exposure is potentially life-threatening.
- Nasogastric aspiration involves the placement of a tube via the nose down into the stomach, the stomach contents are then removed by suction. This procedure is mainly used for liquid ingestions where activated charcoal is ineffective, e.g. ethylene glycol poisoning.
- Whole bowel irrigation cleanses the bowel. This is achieved by giving the patient large amounts of a polyethylene glycol solution. The osmotically balanced polyethylene glycol solution is not absorbed into the body, having the effect of flushing out the entire gastrointestinal tract. Its major uses are to treat ingestion of sustained release drugs, toxins not absorbed by activated charcoal (e.g., lithium, iron), and for removal of ingested drug packets (body packing/smuggling).[12]
Enhanced excretion
A poison is any substance that is harmful to your body. You might swallow it, inhale it, inject it, or absorb it through your skin. Any substance can be poisonous if too much is taken. Poisons can include
The effects of poisoning range from short-term illness to brain damage, coma, and death. To prevent poisoning it is important to use and store products exactly as their labels say. Keep dangerous products where children can't get to them. Treatment for poisoning depends on the type of poison. If you suspect someone has been poisoned, call your local poison control center right away.Alcohol poisoning is a serious — and sometimes deadly — consequence of drinking large amounts of alcohol in a short period of time. Drinking too much too quickly can affect your breathing, heart rate, body temperature and gag reflex and potentially lead to coma and death.
Alcohol poisoning can also occur when adults or children accidentally or intentionally drink household products that contain alcohol.
A person with alcohol poisoning needs immediate medical attention. If you suspect someone has alcohol poisoning, call for emergency medical help right away.
Alcohol poisoning signs and symptoms include:
- Confusion
- Vomiting
- Seizures
- Slow breathing (less than eight breaths a minute)
- Irregular breathing (a gap of more than 10 seconds between breaths)
- Blue-tinged skin or pale skin
- Low body temperature (hypothermia)
- Passing out (unconsciousness) and can't be awakened
It's not necessary to have all these signs and symptoms before you seek help. A person who is unconscious or can't be awakened is at risk of dying.
When to see a doctor
If you suspect that someone has alcohol poisoning — even if you don't see the classic signs and symptoms — seek immediate medical care.
Alcohol poisoning is an emergency
If you're with someone who has been drinking a lot of alcohol and you see any of the signs or symptoms above, here's what to do:
- Call 911 or your local emergency number immediately. Never assume that a person will sleep off alcohol poisoning.
- Be prepared to provide information. If you know, be sure to tell hospital or emergency personnel the kind and amount of alcohol the person drank, and when.
- Don't leave an unconscious person alone. Because alcohol poisoning affects the way your gag reflex works, someone with alcohol poisoning may choke on his or her own vomit and not be able to breathe. While waiting for help, don't try to make the person vomit because he or she could choke.
- Help a person who is vomiting. Try to keep him or her sitting up. If the person must lie down, make sure to turn his or her head to the side — this helps prevent choking. Try to keep the person awake to prevent loss of consciousness.
Don't be afraid to get help
It can be difficult to decide if you think someone is drunk enough to warrant medical intervention, but it's best to err on the side of caution. You may worry about the consequences for yourself or your friend or loved one, particularly if you're underage. But the consequences of not getting the right help in time can be far more serious.
Alcohol in the form of ethanol (ethyl alcohol) is found in alcoholic beverages, mouthwash, cooking extracts, some medications and certain household products. Ethyl alcohol poisoning generally results from drinking too many alcoholic beverages, especially in a short period of time.
Other forms of alcohol — including isopropyl alcohol (found in rubbing alcohol, lotions and some cleaning products) and methanol or ethylene glycol (a common ingredient in antifreeze, paints and solvents) — can cause another type of toxic poisoning that requires emergency treatment.
Binge drinking
A major cause of alcohol poisoning is binge drinking — a pattern of heavy drinking when a male rapidly consumes five or more alcoholic drinks within two hours, or a female downs at least four drinks within two hours. An alcohol binge can occur over hours or last up to several days.
You can consume a fatal dose before you pass out. Even when you're unconscious or you've stopped drinking, alcohol continues to be released from your stomach and intestines into your bloodstream, and the level of alcohol in your body continues to rise.
Poisoning first aid
Poisoning is caused by exposure to a harmful substance. This can be due to swallowing, injecting, breathing in, or other means. Most poisonings occur by accident.
Immediate first aid is very important in a poisoning emergency. The first aid you give before getting medical help can save a person's life.
This is for information only and not for use in the treatment or management of an actual poison exposure.
In the United States, call 1-800-222-1222 to speak with a local poison control center. This hotline number will let you talk to experts in poisoning. They will give you further instructions.
Millions of poisonings are reported to United States poison control centers every year. Many result in death.
It is important to note that just because a package does not have a warning label does not mean a substance is safe. You should consider poisoning if someone suddenly becomes sick for no apparent reason. Poisoning should also be considered if the person is found near a furnace, car, fire, or in an area that is not well ventilated.
Symptoms of poisoning may take time to develop. However, if you think someone has been poisoned, DO NOT wait for symptoms to develop. Get medical help right away.
Items that can cause poisoning include:
- Carbon monoxide gas (from furnaces, gas engines, fires, space heaters)
- Certain foods
- Chemicals in the workplace
- Drugs, including over-the-counter and prescription medicines (such as an aspirin overdose) and illicit drugs such as cocaine
- Household detergents and cleaning products
- Household and outdoor plants (eating toxic plants)
- Insecticides
- Paints
Symptoms vary according to the poison, but may include:
Seek immediate medical help.
For poisoning by swallowing:
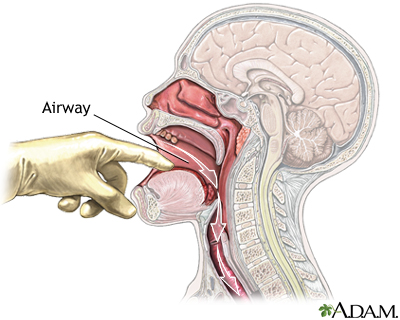
Check and monitor the person's airway, breathing, and pulse. If necessary, begin rescue breathing and CPR.
- Try to make sure that the person has indeed been poisoned. It may be hard to tell. Some signs include chemical-smelling breath, burns around the mouth, difficulty breathing, vomiting, or unusual odors on the person. If possible, identify the poison.
- DO NOT make a person throw up unless told to do so by poison control or a health care professional.
- If the person vomits, clear the person's airway. Wrap a cloth around your fingers before cleaning out the mouth and throat. If the person has been sick from a plant part, save the vomit. It may help experts identify what medicine can be used to help reverse the poisoning.
- If the person starts having convulsions, give convulsion first aid.
- Keep the person comfortable. The person should be rolled onto the left side, and remain there while getting or waiting for medical help.
- If the poison has spilled on the person's clothes, remove the clothing and flush the skin with water.
For inhalation poisoning:
Call for emergency help. Never attempt to rescue a person without notifying others first.
- If it is safe to do so, rescue the person from the danger of the gas, fumes, or smoke. Open windows and doors to remove the fumes.
- Take several deep breaths of fresh air, and then hold your breath as you go in. Hold a wet cloth over your nose and mouth.
- DO NOT light a match or use a lighter because some gases can catch fire.
- After rescuing the person from danger, check and monitor the person's airway, breathing, and pulse. If necessary, begin rescue breathing and CPR.
- If necessary, perform first aid for eye injuries or convulsion first aid.
- If the person vomits, clear the person's airway. Wrap a cloth around your fingers before cleaning out the mouth and throat.
- Even if the person seems perfectly fine, get medical help.
DO NOT:
- Give an unconscious person anything by mouth.
- Induce vomiting unless you are told to do so by the Poison Control Center or a doctor. A strong poison that burns on the way down the throat will also do damage on the way back up.
- Try to neutralize the poison with lemon juice or vinegar, or any other substance, unless you are told to do so by the Poison Control Center or a doctor.
- Use any "cure-all" type antidote.
- Wait for symptoms to develop if you suspect that someone has been poisoned.After doing first aid steps at home, you may need to go to the emergency room. Take the container with you to the hospital, if possible. At the hospital you will have an exam. You also may need the following tests and treatments.
- Activated charcoal
- Airway support, including oxygen, breathing tube through the mouth (intubation),and ventilator (breathing machine)
- Blood and urine tests
- Chest x-ray
- CT (computerized tomography, or advanced imaging) scan
- EKG (electrocardiogram, or heart tracing)
- Fluids through the vein (IV)
- Laxative
- Medicines to treat symptoms, including antidotes to reverse the effects of the poisoning if one exists

