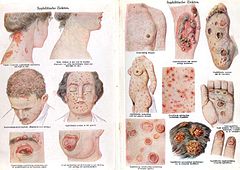
Sexually transmitted diseases (STDs) are infectious diseases thatspread from person to person through intimate contact. STDs can affect guys and girls of all ages and backgrounds who are having sex — it doesn't matter if they're rich or poor.
Many men are quick to assume that if they had a sexually transmitted disease (STD), they would know it. While most STDs do cause symptoms, many are easily mistaken for other conditions. In some cases there are no symptoms at all. Understanding the risks and knowing the signs and symptoms of common STDs in men is crucial for any man who is sexually active.Sexually transmitted infections (STI), also referred to as sexually transmitted diseases (STD) and venereal diseases (VD), are infections that are commonly spread by sex, especially vaginal intercourse, anal sex and oral sex. Most STIs initially do not cause symptoms.[1] This results in a greater risk of passing the disease on to others.[2][3] Symptoms and signs of disease may include vaginal discharge, penile discharge, ulcers on or around the genitals, andpelvic pain. STIs acquired before or during birth may result in poor outcomes for the baby. Some STIs may cause problems with the ability to get pregnant.[1]
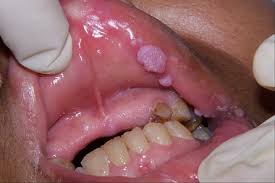
More than 30 different bacteria, viruses, and parasites can cause STIs.[1] Bacterial STIs include chlamydia, gonorrhea, and syphilis among others. Viral STIs include genital herpes, HIV/AIDS, and genital warts among others. Parasitic STIs include trichomoniasis among others. While usually spread by sex, some STIs can also be spread by non-sexual contact with contaminated blood and tissues, breastfeeding, or during childbirth.[1] STI diagnostic tests are easily available in the developed world, but this is often not the case in the developing world.[1]
The most effective way of preventing STIs is by not having sex.[4] Some vaccinations may also decrease the risk of certain infections including hepatitis Band some types of HPV.[4] Safer sex practices such as use of condoms, having a smaller number of sexual partners, and being in a relationship where each person only has sex with the other also decreases the risk.[1][4] Circumcision in males may be effective to prevent some infections.[1] Most STIs are treatable or curable.[1] Of the most common infections, syphilis, gonorrhea, chlamydia, trichomoniasis are curable, while herpes, hepatitis B, HIV/AIDS, and HPV are treatable but not curable.[1] Resistance to certain antibiotics is developing among some organisms such as gonorrhea.[5]
Most Common STDs for Women and MEN
When you're planning for a hot night under the sheets, you might not want to think about STDs. If you're happily smitten with your long-time partner, you may not think you have to.
But the possibility of infections and diseases are as much a part of sex as the fun is. Both men and women get them. Even if you didn't realize it, you've probably had an STD.
Knowledge is power when it comes to your sexual health. Recognizing the symptoms is a start, but you won't always notice chlamydia,gonorrhea, herpes, and other STDs. You'll need to get tested to protect yourself -- and your partner. Fortunately, all of these common STDs can be treated, and most can be cured.
Classification
Until the 1990s,[citation needed] STIs were commonly known as venereal diseases, the word venereal being derived from the Latin word venereus, and meaning relating to sexual intercourse or desire, ultimately derived from Venus, the Roman goddess of love.[10] "Social disease" was a phrase used as a euphemism.
The World Health Organization (WHO) has recommended sexually transmitted infection as the preferred term since 1999.[9] Sexually transmitted infection is a broader term than sexually transmitted disease.[11] An infection is a colonization by a parasitic species, which may not cause any adverse effects. In a disease, the infection leads to impaired or abnormal function. In either case, the condition may not exhibit signs or symptoms. Increased understanding of infections like HPV, which infects a significant portion of sexually active individuals but cause disease in only a few, has led to increased use of the term STI. Public health officials originally introduced the term sexually transmitted infection, which clinicians are increasingly using alongside the term sexually transmitted disease in order to distinguish it from the former.[12]
STD may refer only to infections that are causing diseases, or it may be used more loosely as a synonym for STI. Most of the time, people do not know that they are infected with an STI until they are tested or start showing symptoms of disease. Moreover, the term sexually transmissible disease is sometimes used since it is less restrictive in consideration of other factors or means of transmission. For instance, meningitis is transmissible by means of sexual contact but is not labeled an STI because sexual contact is not the primary vector for the pathogens that cause meningitis. This discrepancy is addressed by the probability of infection by means other than sexual contact. In general, an STI is an infection that has a negligible probability of transmission by means other than sexual contact, but has a realistic means of transmission by sexual contact (more sophisticated means—blood transfusion, sharing of hypodermic needles—are not taken into account). Thus, one may presume that, if a person is infected with an STI, e.g., chlamydia, gonorrhea, genital herpes, HPV it was transmitted to him/her by means of sexual contact.
Signs and symptoms
Not all STIs are symptomatic, and symptoms may not appear immediately after infection. In some instances a disease can be carried with no symptoms, which leaves a greater risk of passing the disease on to others. Depending on the disease, some untreated STIs can lead to infertility, chronic pain or even death.[13]
The presence of an STI in prepubescent children may indicate sexual abuse.[14]


Cause
Transmission
The risks and transmission probabilities of sexually transmitted diseases are summarized by act in the table:[15][16][17][18][19][20][21][22][23][24][25][26][27]
Bacterial
Fungal
Viral
- Viral hepatitis (Hepatitis B virus)—saliva, venereal fluids.
(Note: Hepatitis A and Hepatitis E are transmitted via the fecal-oral route; Hepatitis C is rarely sexually transmittable,[41] and the route of transmission ofHepatitis D (only if infected with B) is uncertain, but may include sexual transmission.[42][43][44]) - Herpes simplex (Herpes simplex virus 1, 2) skin and mucosal, transmissible with or without visible blisters
- HIV (Human Immunodeficiency Virus)—venereal fluids, semen, breast milk, blood
- HPV (Human Papillomavirus)—skin and mucosal contact. 'High risk' types of HPV cause almost all cervical cancers, as well as some anal, penile, and vulvar cancer. Some other types of HPV cause genital warts.
- Molluscum contagiosum (molluscum contagiosum virus MCV)—close contact
Parasites
Protozoal
Main types
Sexually transmitted infections include:
- Chlamydia is a sexually transmitted infection caused by the bacterium Chlamydia trachomatis. In women, symptoms may include abnormal vaginal discharge, burning during urination, and bleeding in between periods, although most women do not experience any symptoms.[45] Symptoms in men include pain when urinating, and abnormal discharge from their penis.[46] If left untreated in both men and women, Chlamydia can infect the urinary tract and potentially lead to pelvic inflammatory disease (PID). PID can cause serious problems during pregnancy and even has the potential to cause infertility. It can cause a woman to have a potentially deadly ectopic pregnancy, in which the child is born outside of the uterus. However, Chlamydia can be cured with antibiotics.
- The two most common forms of herpes are caused by infection with herpes simplex virus (HSV). HSV-1 is typically acquired orally and causes cold sores, HSV-2 is usually acquired during sexual contact and affects the genitals, however either strain may affect either site.[47] Some people are asymptomatic or have very mild symptoms. Those that do experience symptoms usually notice them 2 to 20 days after exposure which last 2 to 4 weeks. Symptoms can include small fluid-filled blisters, headaches, backaches, itching or tingling sensations in the genital or anal area, pain during urination, Flu like symptoms, swollen glands, or fever. Herpes is spread through skin contact with a person infected with the virus. The virus affects the areas where it entered the body. This can occur through kissing, vaginal intercourse, oral sex or anal sex. The virus is most infectious during times when there are visible symptoms, however those who are asymptomatic can still spread the virus through skin contact.[48] The primary attack is the most severe because the body does not have any antibodies built up. After the primary attack, one might have recurring attacks that are milder or might not even have future attacks. There is no cure for the disease but there are antiviral medications that treat its symptoms and lower the risk of transmission (Valtrex). Although HSV-1 is typically the "oral" version of the virus, and HSV-2 is typically the "genital" version of the virus, a person with HSV-1 orally CAN transmit that virus to their partner genitally. The virus, either type, will settle into a nerve bundle either at the top of the spine, producing the "oral" outbreak, or a second nerve bundle at the base of the spine, producing the genital outbreak.
- The human papillomavirus (HPV) is the most common STI in the United States.[49] There are more than 40 different strands of HPV and many do not cause any health problems. In 90% of cases the body’s immune system clears the infection naturally within 2 years.[50] Some cases may not be cleared and can lead to genital warts (bumps around the genitals that can be small or large, raised or flat, or shaped like cauliflower) or cervical cancer and other HPV related cancers. Symptoms might not show up until advanced stages. It is important for women to get pap smears in order to check for and treat cancers. There are also two vaccines available for women (Cervarix and Gardasil) that protect against the types of HPV that cause cervical cancer. HPV can be passed through genital-to-genital contact as well as during oral sex. It is important to remember that the infected partner might not have any symptoms.
- Gonorrhea is caused by bacterium that lives on moist mucous membranes in the urethra, vagina, rectum, mouth, throat, and eyes. The infection can spread through contact with the penis, vagina, mouth or anus. Symptoms of Gonorrhea usually appear 2 to 5 days after contact with an infected partner however, some men might not notice symptoms for up to a month. Symptoms in men include burning and pain while urinating, increased urinary frequency, discharge from the penis (white, green, or yellow in color), red or swollen urethra, swollen or tender testicles, or sore throat. Symptoms in women may include vaginal discharge, burning or itching while urinating, painful sexual intercourse, severe pain in lower abdomen (if infection spreads to fallopian tubes), or fever (if infection spreads to fallopian tubes), however many women do not show any symptoms.[51] There are some antibiotic resistant strains for Gonorrhea but most cases can be cured with antibiotics.
- Syphilis is an STI caused by a bacterium. Untreated, it can lead to complications and death.[52] Clinical manifestations of syphilis include the ulceration of the uro-genital tract, mouth or rectum; if left untreated the symptoms worsen. In recent years, the prevalence of syphilis has declined in Western Europe, but it has increased in Eastern Europe (former Soviet states). A high incidence of syphilis can be found in places such as Cameroon, Cambodia, Papua New Guinea.[53] Syphilis infections are increasing in the United States.[54]
- Trichomoniasis is a common STI that is caused by infection with a protozoan parasite called Trichomonas vaginalis.[55] Trichomoniasis affects both women and men, but symptoms are more common in women.[56] Most patients are treated with an antibiotic called metronidazole, which is very effective.[57]
- HIV (human immunodeficiency virus) damages the body's immune system, which interferes with its ability to fight off disease-causing agents. The virus kills CD4 cells, which are white blood cells that help fight off various infections. HIV is carried in body fluids, and is spread by sexual activity. It can also be spread by contact with infected blood, breast feeding, childbirth, and from mother to child during pregnancy.[58] When HIV is at its most advanced stage, an individual is said to have AIDS (acquired immunodeficiency syndrome).[59] There are different stages of the progression of and HIV infection. The stages include primary infection, asymptomatic infection, symptomatic infection, and AIDS. In the primary infection stage, an individual will have flu like symptoms (headache, fatigue, fever, muscle aches) for about 2 weeks. In the asymptomatic stage, symptoms usually disappear, and the patient can remain asymptomatic for years. When HIV progresses to the symptomatic stage, the immune system is weakened, and has a low cell count of CD4+ T Cells. When the HIV infection becomes life-threatening, it is called AIDS. People with AIDS fall prey to opportunistic infections and die as a result.[45] When the disease was first discovered in the 1980s, those who had AIDS were not likely to live longer than a few years. There are now antiretroviral drugs (ARVs) available to treat HIV infections. There is no known cure for HIV or AIDS but the drugs help suppress the virus. By suppressing the amount of virus in the body, people can lead longer and healthier lives. Even though their virus levels may be low they can still spread the virus to others.[60]
Unscreened
There are many species of bacteria, protozoa, fungi, and viruses, many which remain undocumented or poorly studied with regards to sexual transmission.[citation needed] Despite that the above include what are generally known as STIs, sexually transmission of microbes is far from limited to the above list. Since the sexual route of transmission is not considered common, and/or the microbe itself is not implicated in a major research study on disease, the following pathogens are simply not screened for in sexual health clinics. Some of these microbes are known to be sexually transmittable.
Microbes known to be sexually transmissible (but not generally considered STDs/STIs) include:
Pathophysiology
Many STIs are (more easily) transmitted through the mucous membranes of the penis, vulva, rectum, urinary tract and (less often—depending on type of infection) the mouth, throat, respiratory tract andeyes.[63] The visible membrane covering the head of the penis is a mucous membrane, though it produces no mucus (similar to the lips of the mouth). Mucous membranes differ from skin in that they allow certain pathogens into the body.[64] The amount of contact with infective sources which causes infection varies with each pathogen but in all cases a disease may result from even light contact from fluid carriers like venereal fluids onto a mucous membrane.
This is one reason that the probability of transmitting many infections is far higher from sex than by more casual means of transmission, such as non-sexual contact—touching, hugging, shaking hands—but it is not the only reason. Although mucous membranes exist in the mouth as in the genitals, many STIs seem to be easier to transmit through oral sex than through deep kissing. According to a safe sex chart, many infections that are easily transmitted from the mouth to the genitals or from the genitals to the mouth are much harder to transmit from one mouth to another.[65] With HIV, genital fluids happen to contain much more of the pathogen than saliva. Some infections labeled as STIs can be transmitted by direct skin contact. Herpes simplex and HPV are both examples. KSHV, on the other hand, may be transmitted by deep-kissing but also when saliva is used as a sexual lubricant.
Depending on the STI, a person may still be able to spread the infection if no signs of disease are present. For example, a person is much more likely to spread herpes infection when blisters are present than when they are absent. However, a person can spread HIV infection at any time, even if he/she has not developed symptoms of AIDS.
All sexual behaviors that involve contact with the bodily fluids of another person should be considered to contain some risk of transmission of sexually transmitted diseases. Most attention has focused on controlling HIV, which causes AIDS, but each STI presents a different situation.
As may be noted from the name, sexually transmitted diseases are transmitted from one person to another by certain sexual activities rather than being actually caused by those sexual activities.Bacteria, fungi, protozoa or viruses are still the causative agents. It is not possible to catch any sexually transmitted disease from a sexual activity with a person who is not carrying a disease; conversely, a person who has an STI got it from contact (sexual or otherwise) with someone who had it, or his/her bodily fluids. Some STIs such as HIV can be transmitted from mother to child either during pregnancy or breastfeeding.
Although the likelihood of transmitting various diseases by various sexual activities varies a great deal, in general, all sexual activities between two (or more) people should be considered as being a two-way route for the transmission of STIs, i.e., "giving" or "receiving" are both risky although receiving carries a higher risk.
Healthcare professionals suggest safer sex, such as the use of condoms, as the most reliable way of decreasing the risk of contracting sexually transmitted diseases during sexual activity, but safer sex should by no means be considered an absolute safeguard. The transfer of and exposure to bodily fluids, such as blood transfusions and other blood products, sharing injection needles, needle-stick injuries (when medical staff are inadvertently jabbed or pricked with needles during medical procedures), sharing tattoo needles, and childbirth are other avenues of transmission. These different means put certain groups, such as medical workers, and haemophiliacs and drug users, particularly at risk.
Recent epidemiological studies have investigated the networks that are defined by sexual relationships between individuals, and discovered that the properties of sexual networks are crucial to the spread of sexually transmitted diseases. In particular, assortative mixing between people with large numbers of sexual partners seems to be an important factor.
It is possible to be an asymptomatic carrier of sexually transmitted diseases. In particular, sexually transmitted diseases in women often cause the serious condition of pelvic inflammatory disease
Chlamydia
Chlamydia is a bacterial STD that is transmitted during anal, oral, or vaginal sex with someone who is infected with chlamydia. It is one of the most common STDs in the United States. According to the Centers for Disease Control and Prevention (CDC), 1,401,906 chlamydia infections were reported in the United States in 2013.
Many people who become infected with chlamydia don’t ever display symptoms. Others only begin to display symptoms several weeks after becoming infected. Some of the symptoms of chlamydia in men include:
- pain when urinating
- penile discharge
- swollen testicles

Gonorrhea
Gonorrhea is a bacterial infection that can affect the anus, throat, or urethra. It is transmitted during anal, oral, or vaginal sex with a man or woman who has been infected. Most men with gonorrhea don’t display any symptoms at all. For those who do, symptoms include:
- pain when urinating
- a green, white, or yellow discharge from the penis
- swollen testicles
Hepatitis B
Hepatitis B is a form of hepatitis that is caused by the hepatitis B virus (HBV). Unlike other common STDs that can produce more obvious symptoms focused around the genitals that we tend to associate with STDs, hepatitis B causes a dangerous inflammation of the liver. You can contract hepatitis by coming into contact with the blood or bodily fluids of a person who is infected with the virus.
Many people infected with hepatitis B will not display symptoms at all. Those who do, often mistake symptoms for a cold or the flu. Even if a person has no symptoms, the virus can continue to damage the liver if it’s left untreated. Hepatitis B symptoms include:
- loss of appetite
- feeling lethargic
- low-grade fever
- muscle and joint pain and aches
- nausea
- vomiting
- jaundice (yellow hue to the skin and dark urine)
Herpes (Simplex)
Herpes is a viral infection that is caused by the herpes simplex virus (HSV). Herpes may affect the mouth (oral herpes or HSV Type 1) or the genitals (genital herpes or HSV Type 2). Herpes is transmitted through direct contact with the mouth or genitals of a person who has been infected with the virus through sexual intercourse or oral sex and kissing.
The symptoms of herpes can be difficult to spot. Many people won’t have any symptoms at all. Those who do will develop blisters that are often mistaken for other skin conditions like pimples. Symptoms often occur between two days and two weeks after infection. The initial outbreak can be severe. Common symptoms of herpes in men are:
- tingling, itching, or burning of the skin in the area where the blisters will appear
- blisters on the penis, testicles, on and around the anus, buttocks, or thighs
- blisters on the lips, tongue, gums, and other parts of the body
- aching muscles in the lower back, buttocks, thighs, or knees
- swollen and sometimes tender lymph nodes in the groin
- loss of appetite
- fever
- feeling unwell
Human Papillomavirus (HPV)
HPV is a term used to refer to a group of viruses that comprises more than 150 strains. While most of these strains are quite harmless, 40 are considered potentially harmful. These are classified as being either low-risk or high-risk strains. HPV is one of the most common sexually transmitted diseases today. Most men and women will eventually acquire one strain of the virus during his or her lifetime. According to the CDC, there are approximately 14 million new cases of HPV every year. Currently there are at least 79 million people infected with HPV in the United States.
The low-risk strains may result in genital warts in some people, while in men the high-risk strains could lead to cancers of the anus, throat, and penis. HPV can be transmitted through skin-to-skin contact with a person who has been infected with the virus and is most commonly transmitted through anal, oral, or vaginal sex.
Most men infected with HPV won’t have any symptoms at all, but those who do have symptoms may have:
- genital warts (flat and flesh-colored or clusters of tiny bumps described as having a cauliflower appearance)
- warts in the mouth or throat (spread through oral sex with an infected partner)
Unlike other STDs which can only be prevented through the use of condoms or by abstinence, HPV can now be prevented with vaccines. There are two HPV vaccines that have been approved by the FDA: Gardasil and Cervarix. They are both effective in the prevention of HPV types 16 and 18 that are high risk and responsible for causing most cervical cancers (70 percent) and types 6 and 11 that cause over 90 percent of genital warts. A new version of Gardasil, called Gardasil 9, protects against five more strains of the virus. Gardasil 9 was approved by the U.S. Food and Drug Administration in December 2014. It’ll eventually replace the older version.
Though originally recommended only for females age 11 to 26, Gardasil has now also been licensed for use in boys and men age 11 to 21 to prevent genital warts.
Syphilis
Syphilis is a bacterial STD that can be transmitted through anal, oral, or vaginal sex. This ancient disease is still quite prevalent today. Syphilis is considered one of the more serious STDs in men because of its link to HIV and the increased risk of developing HIV when infected with syphilis.
Syphilis has four different phases: primary, secondary, latent, and tertiary. Each phase has its own set of symptoms. The symptoms of primary syphilis in men may include:
- a very small, firm, and painless sore where the bacteria entered the body, usually on the penis, anus, or lips
- swollen lymph nodes in the area near the sore
Symptoms of secondary syphilis may include:
- a skin rash that does not itch, commonly found on the palms of the hands or soles of the feet
- tiredness
- sore throat
- headache
- swollen lymph nodes
Latent syphilis is the stage that occurs after the symptoms of secondary have stopped and the STD has gone untreated. Tertiary syphilis is the fourth stage. It’s rare as few people actually enter the fourth stage even when the syphilis is left untreated. It can cause serious complications, including damage to the heart, nervous system, brain, joints, and other parts of the body. Syphilis can cause serious medical issues and death if it reaches this stage, even several years after infection.
Sexually Transmitted Infections (STIs): Types,
Symptoms
Sexually Transmitted Infections (STIs), also known as Sexually
Transmitted Diseases (STDs) or Venereal Diseases (VD) are diseases that are
passed on from one person to another through sexual contact, and sometimes by
genital contact - the infection can be passed on via vaginal intercourse, oral
sex, and anal sex.
Some sexually
transmitted infections can spread through the use of unsterilized IV drug
needles, from mother to baby during childbirth or breastfeeding, and blood
transfusions.
Sexually transmitted
infections have been around for thousands of years.
Microorganisms that
exists on the skin or mucus membranes of the male or female genital area can be
transmitted, as can organisms in semen, vaginal secretions or blood during
sexual intercourse.

Common types of STI/STD
The term "venereal
disease" is much less used today, while "sexually transmitted
diseases" is slowly giving way to "sexually transmitted
infections", because the last term has a broader range of meaning - a
person can pass on the infection without having a disease (they do not have to
be ill to infect other people).
The genital areas are
generally moist and warm environments - ideal for the proliferation of yeasts,
viruses and bacteria.
Examples of sexually
transmitted infections (STIs) include:
§ Chlamydia
§ Chancroid
§ Crabs (Pubic
Lice)
§ Genital herpes
§ Genital warts
§ Hepatitis
B
§ HIV/AIDS
§ Human
Papillomavirus (HPV)
§ Trichomoniasis
(parasitic infection)
§ Molluscum
Contagiosum
§ Pelvic
Inflammatory Disease (PID)
§ Scabies
§ Syphilis
§ Syphilis, gonorrhea
§ Trichomoniasis
(Trich)
§ Yeast
infections
Sexually transmitted
infections are more easily passed on during unprotected sex - without using a
condom.
Some infections can be passed on via sexual contact, but are not
classed as sexually transmitted infections, because sexual contact is not the
primary vector for the pathogens that cause the infections - an example is meningitis,
it can be passed on via sexual contact, but usually people become infected for
other reasons.
The WHO (World Health
Organization) estimated over ten years ago that over 1 million people each day
became infected with a sexually transmitted infection - most experts believe the
figure is considerably higher today. The majority of these new infections occur
in young adults aged up to 25 years, while approximately one third occur among
individuals younger than 20 years of age. Globally, girls aged 14 to 19 are
almost twice as susceptible to STIs than boys of the same age.
Common
sexually transmitted infections
We take a look at some
of the most common sexually transmitted infections below.
1)
Chlamydia

There are nearly 3 million
reported cases of Chlamydia in the US each year (American Sexual Health
Association).
Also known as chamydial
infection, Chlamydia is an STI caused by Chlamydia
trachomatis (C. trachomatis), a bacterium that infects humans exclusively.
Chlamydia is the most common infectious cause of genital and eye diseases
globally - it is also the leading bacterial STI.
According to the CDC
(Centers for Disease Control and Prevention), 6.8% of girls aged 14 to 19 years
have Chlamydia today.
Women with Chlamydia do
not usually have signs or symptoms. If there are any, they are usually
non-specific and may include:
§ Cystitis
§ A
change in vaginal discharge
§ Mild
lower abdominal pain
If the Chlamydia is left
untreated, it may lead to the following signs and symptoms
§ Pelvic
pain
§ Painful
sexual intercourse, either intermittently or all the time
§ Bleeding
between menstrual periods
You can learn more about chlamydia here.
2)
Chancroid
Also known as soft
chancre and ulcus molle. A bacterial infection caused by fastidious
Gram-negative streptobacillus Haemophilus
ducreyi, and is characterized by painful sores on the genitalia. It is
spread solely through sexual contact.
Infection rates are very
low in rich countries; it is more common in developing nations, especially
among commercial sex workers and some low socioeconomic groups.
The average prevalence
in the US, UK, Australia, France and Canada is approximately 1 case in every 2
million people. It is a risk factor for contracting HIV, due to their
shared-risk exposure; also, one infection facilitates the transmission of the
other
Within one day to two
weeks after becoming infected, the patient develops a bump that turns into an
ulcer within a day. The ulcer can be from 1/8 of an in to 2 inches across, it
is very painful, may have well defined, undermined borders, has a
yellowish-gray material at its base. If the base is grazed it will typically
bleed. In about 30% to 60% of cases, the lymph nodes swell and become painful
(lymphadenopathy).
Women often have at
least four ulcers, while men usually have just one. Males tend to have fewer
and less severe symptoms. The ulcers typically appear at the groove at the back
of the glans penis (coronal sulcus) in uncircumcised males, or the labia minora
or fourchette in females.
Chancroid is treated
with a seven day course of Erythromycin, a single oral 1 gram dose of
Azithromycin, or a single IM dose of Ceftriaxone.
3) Crabs
(Pubic Lice)
Pthiriasis (pubic lice
manifestations) are primarily spread through sexual contact. Pets do not play
any part in the transmission of human lice. The lice attach to the pubic hair,
and may also be sometimes found in the armpits, moustache, beard, eyelashes,
and eyebrows. They feed on human blood.
The vernacular
"crabs" comes from the appearance of the lice, with their crab-like
claws and body shape.
4)
Genital herpes
This STI is caused by
the herpes simples virus (HSV). The virus affects the skin, cervix, genitals,
and some other parts of the body. There are two types:
§ HSVp1,
also known as Herpes Type 1
§ HSV-2,
also known as Herpes Type 2.
Herpes is a long-term
(chronic) condition. A significant number of infected individuals never show
any symptoms and do not know about their herpes status.
HSV is easily
transmissible from human-to-human - by direct contact. Most commonly,
transmission occurs through vaginal, oral or anal sex. In most cases, the virus
remains dormant after entering a human being.
The signs and symptoms
associated with genital herpes, if they do appear, may include:
§ Blisters
and ulceration on the cervix
§ Vaginal
discharge
§ Pain on
urinating
§ Fever
§ Generally
feeling unwell (malaise)
§ Cold
sores around the
mouth
§ Red
blisters - these can be painful, especially after they burst and leave ulcers
on the external genital area, rectum, thighs and buttocks.
You can learn more about genital herpes here.
On the next page we look at other common
sexually transmitted infections including
Hepatitis B, HIV/AIDS, Human Papillomavirus, Trichomoniasis, Scabies, Syphilis,
Gonorrhea and more. On the final page we look at the best ways to prevent
getting a sexually transmitted infection.
5) Hepatitis B
This STI is caused by
the Hepatitis B Virus (HBV). It is transmitted via contact with infected semen,
blood and some other body fluids. A person can become infected by having
unprotected sex, using an unsterilized syringe, being accidentally pricked by a
sharp object, drinking infected breast milk, or being bitten by an infected
person.
The patient's liver swells and he/she can suffer serious liver
damage as a result of the infection, which can eventually lead to cancer. In some
cases, the disease can become chronic. Blood donation centers always check to
make sure the donor's blood is free of thehepatitis
B virus.
You can learn more about hepatitis here.
6)
HIV/AIDS
HIV (Human
Immunodeficiency Virus) is the virus that causes AIDS (Acquired Immune
Deficiency Syndrome or Acquired Immunodeficiency Syndrome). Put simply, HIV is
the virus while AIDS is the illness/disease. When a person has AIDS, their
immune system is altered, and they become much more vulnerable to infections
and diseases. As the disease progresses, this susceptibility worsens.
HIV exists in the body
fluids of infected people, such as semen, blood, breast milk and vaginal
fluids. HIV can be transmitted through blood-to-blood contact, which may occur
during sexual contact (vaginal oral or anal sex), blood transfusions,
breastfeeding, childbirth, and the sharing of infected needles.
You can learn more about HIV/AIDS here.
7) Human
Papillomavirus (HPV)
Human Papillomavirus is
a name for a group of viruses that affect the skin, as well as the moist
membranes that line the body, such as the throat, cervix, anus and mouth. There
are over 100 types of HPV, of which about 40 can affect the genital areas of
males and females; these types may also infect the mouth and throat. The ones
that affect the genital area are known as genital
human papillomavirus.
HPV infection can lead
to:
§ The
abnormal growth and alteration of cells within the cervix, which can
significantly increase the risk of developing cancer of the cervix
§ Genital
warts, the most common STI in the majority of developed nations
The majority of infected
individuals have no symptoms and are unaware.

The HPV vaccine prevents HPV
infection
HPV is most commonly
transmitted through vaginal or anal sex. However, oral sex and
genital-to-genital contact (without penetration) are also avenues for
transmission. Infected people with no signs and symptoms can infect others.
An infected pregnant
mother can transmit the virus to her baby during childbirth, although this is very
rare.
According to the CDC,
half of all Americans who are sexually active will become infected with genital
human HPV some time in their lives.
The best way to be
protect from HPV infection is to be vaccinated.
8)
Trichomoniasis
Trichomoniasis is a
common sexually transmitted disease that can affect both males and females.
However, women are more likely to experience symptoms. The infection is caused
by a single-celled protozoan parasite, Trichomonas
vaginalis.
For women, the most
common site of infection is the vagina, while for men it is the urethra (urine
canal). Transmission may occur either by penis-to-vagina sexual intercourse or
vulva-to-vulva contact.
While women may be
infected from either male or female sexual partners, men nearly always become
from having sex with women (not men).
Signs and symptoms of
trichomoniasis include:
§ Vaginal
odor
§ Vaginal
discharge
§ Pain or
discomfort during sexual intercourse
§ Pain
when urinating
A woman with
trichomoniasis is more likely to become HIV infected if she is exposed to the
virus. A woman with trichomoniasis and HIV is also more likely to pass the HIV
onto other sexual partners.
9)
Molluscum Contagiosum
Molluscum Contagiosum is
a contagious skin infection caused by a virus called molluscum contagiosum. There
are four types: MCV-1 (most common), MCV-2 (most commonly sexually transmitted
one), MCV-3, and MCV-4. When it infects young children it is not considered an
STI.
Signs and symptoms
include small, round bumps and indents on the skin. If left untreated, the
bumps usually go away, but this can take up to two years. A health care
provider can remove the bumps with chemicals, an electrical current, or by
freezing them. There are some prescription medicines that will eventually get
rid of the growths.
You can learn more about Molluscum Contagiosum here.
10)
Pelvic Inflammatory Disease (PID)
Pelvic Inflammatory Disease is a broad term for inflammation of the uterus, ovaries, or fallopian
tubes. The disease can eventually lead to scar formation and fibrous brands
that form between tissues and organs. In most cases, PID is caused by a vaginal
or cervical infection, which then spreads. PID can be caused by bacteria,
fungi, or parasites - in the majority of cases the cause is a bacterium.
STIs are the most common
causes of PIDs. However, PIDs may also be a consequence of abortion,
miscarriage, childbirth, or using an intrauterine device. Chlamydia and
gonorrhea are common causes of PID.
Untreated PID can lead to chronic persistent pelvic pain,
ectopic pregnancy, and infertility.
Many females with PID
have no signs or symptoms. Some women find out after seeing a doctor for an
infertility problem. PID caused by Chlamydia usually has no symptoms.
If signs and symptoms do
appear, they may include:
§ Lower
abdominal pain, this may sometimes be severe
§ Fever
§ Fatigue
§ Oligomenorrhea (irregular
periods)
§ Lower back
pain
§ Pain
during sexual intercourse
§ Rectal
pain
§ Change
in vaginal discharge
§ Nausea
and vomiting
You can learn more about Pelvic Inflammatory Disease here.
On the final page we look at other common sexually transmitted infections
including Scabies, Syphilis and Gonorrhea. We also discuss the best methods of
preventing sexually transmitted infections
11) Scabies
Scabies is a contagious
skin condition caused by Sarcoptes
scabiei, a tiny mite. They burrow into the skin and lay their eggs. The
patient develops a skin rash and experiences intense itchiness. Sufferers are
often unaware of their condition for several weeks after initial infection,
which means scabies infestations spread rapidly.
Some experts believe
scabies is caused by poor living conditions and a lack of personal hygiene -
however, there is no scientific proof of this.
Scabies is most commonly
transmitted through close body contact, such as holding hands for a long time
or sexual intercourse. Hugging infected people or simply shaking hands with
them is unlikely to lead to transmission.
The scabies mite cannot
jump or fly. However, it can survive for one or two days after leaving the
human body - this means that sharing clothing or bedding with an infected
person raises the risk of infection. However, prolonged physical contact, as
may occur during sexual intercourse, is the most common route of transmission.
Signs and symptoms of
scabies may not become apparent for several weeks after initial infection, and
may include:
§ A skin
rash - small red spots, known as burrow marks; they look like tiny insect
bites. Some people may think it is eczema.
§ Intense
itching, which gets worse at night or after taking a hot shower
§ The
burrow marks, which typically appear as a small line of at least four tiny
spots, appear on the elbows, wrists, around the nipples (in women), near the
genitals (in men), and in between the toes and fingers.
§ Upon
scratching areas of skin where the rash is, the area can become inflamed and
crusty sores may develop.
§ Less
commonly the rash may appear on the buttocks, ankles, axillae (armpits),
genitalia (in women), groin, the inside of the elbow, scalp, neck, face, head,
shoulders, waist, soles of the feet, lower leg, and knees.
You can learn more about scabies here.
12)
Syphilis
Syphilis is the result
of infection by Treponema
pallidum, a bacterium. It is transmitted by sexual contact - the infected
person has a syphilis lesion. An infected mother can pass on this STI to her
baby during pregnancy, which can result in stillbirth or serious birth defects.
An infected person, when exposed to HIV, has a higher risk of becoming
HIV-positive.
There is a 9 to 90 day
incubation period after initial infection - average time 21 days, before the
initial signs and symptoms of the disease emerge. Each syphilis stage has
characteristic signs and symptoms. Some infected people have no signs, while
for others they may be mild. In some cases, even if signs and symptoms go away,
the bacterium is still there and can cause serious health problems later on.
You can learn more about syphilis here.
13)
Gonorrhea
Also known as the clap or the
drip, this sexually transmitted bacterial infection usually attacks the
mucous membranes. Gonorrhea is the second most common STI in the USA, after
Chlamydia. The bacterium, which is highly contagious, resides in the warm and
moist cavities of the body.
The majority of infected women show no signs or symptoms. If
left untreated, females may develop pelvic inflammatory disease, while males may
develop inflammation of the prostate gland, urethra, or epididymis.
The disease is caused by
the proliferation of Neisseria
gonorrhoeae. The disease can survive in the vagina, penis, mouth, rectum,
or eye; it can be transmitted in a variety of sexual contacts.
As soon as a person is
infected, he/she risks spreading the bacteria to other parts of their body -
somebody may inadvertently rub their eye and spread the infection; this
prolongs the treatment period. A mother can pass the infection on to her baby
during childbirth.
Signs and symptoms of
gonorrhea may appear from two to ten days after initial infection, in some
cases it may take 30 days. Some patients have such mild symptoms that their
infection is mistaken for something else, such as a yeast infection.
Males may have the
following signs and symptoms:
§ Burning
during urination
§ Testicular
pain and/or swelling
§ A
green, white or yellow discharge from the penis
Women are more likely to
show no symptoms, if they do, they may include:
§ Spotting
after sexual intercourse
§ Swelling
of the vulva (vulvitis)
§ Irregular
bleeding (between periods)
§ Pink
eye (conjunctivitis)
§ Pain in
the pelvic area
§ Burning
or pain during urination
If the rectum becomes infected, there may be anal itching, painful bowel movements, and
sometimes discharge. When transmission occurred from oral sex, there may be
burning sensation in the throat and swollen glands.
You can learn more about gonorrhea here.
Prevention
of sexually transmitted infections
Have "safe sex" - for each sexual act, use a new latex condom, whether it be
oral, vaginal or anal sex. Avoid using an oil-based lubricant, such as
petroleum jelly when using a latex condom. Non-barrier forms of contraception do nothing to protect people from
sexually transmitted infections. Examples include oral contraceptives or
intrauterine devices.

Using a condom is one of the
best methods of STI prevention.
Abstain - abstaining from any sexual act is probably the most effective
way to avoid becoming infected with an STI.
Be faithful to one
uninfected partner - be in a long-term
relationship with a person who is not infected, and remain faithful.
Vaccinations - there are vaccinations which can protect from eventually
developing some types of cancer caused by two STIs - the HPV (human
papillomavirus) and Hepatitis B vaccines.
Check for infections - before sexual intercourse with a new partner, check that the
partner and yourself have no STIs.
Drink alcohol in
moderation - people who are drunk are more likely to
engage in risky behavior. Avoid using some recreational drugs which may also
affect judgment.
Explain you want safe
sex - before engaging in any sexual act with a new partner, make it
clear that you would only consider safe sex.
Education - parents and schools need to teach children about the
importance of safe sex, and explain how to prevent becoming infected with an
STI. This should also include explaining that the safest protection is to wait
to have sex.Prevention is key in addressing incurable STIs, such as HIV and herpes. Sexual health clinics promote the use of condoms and provide outreach for at-risk communities.
The most effective way to prevent sexual transmission of STIs is to avoid contact of body parts or fluids which can lead to transfer with an infected partner. Not all sexual activities involve contact: cybersex, phonesex or masturbation from a distance are methods of avoiding contact. Proper use of condoms reduces contact and risk. Although a condom is effective in limiting exposure, some disease transmission may occur even with a condom.[66]
Both partners should get tested for STIs before initiating sexual contact, or before resuming contact if a partner engaged in contact with someone else. Many infections are not detectable immediately after exposure, so enough time must be allowed between possible exposures and testing for the tests to be accurate. Certain STIs, particularly certain persistent viruses like HPV, may be impossible to detect with current medical procedures.
Many diseases that establish permanent infections can so occupy the immune system that other diseases become more easily transmitted. The innate immune system led by defensins against HIV can prevent transmission of HIV when viral counts are very low, but if busy with other viruses or overwhelmed, HIV can establish itself. Certain viral STI's also greatly increase the risk of death for HIV infected patients.
Strategies to increase testing for HIV and STIs have proved to be successful. Some treatment facilities utilize in-home test kits and have the person return the test for follow-up. Other facilities strongly encourage that those previously infected return to ensure that the infection has been eliminated. Novel strategies to foster re-testing have been the use of text messaging and email as reminders. These types of reminders are now used in addition to phone calls and letters.[67]
Vaccines
Vaccines are available that protect against some viral STIs, such as Hepatitis A, Hepatitis B, and some types of HPV. Vaccination before initiation of sexual contact is advised to assure maximal protection. The development of vaccines to protect against gonorrhea is ongoing.[68]
Condoms
Condoms and female condoms only provide protection when used properly as a barrier, and only to and from the area that it covers. Uncovered areas are still susceptible to many STIs.
In the case of HIV, sexual transmission routes almost always involve the penis, as HIV cannot spread through unbroken skin; therefore, properly shielding the penis with a properly worn condom from the vagina or anus effectively stops HIV transmission. An infected fluid to broken skin borne direct transmission of HIV would not be considered "sexually transmitted", but can still theoretically occur during sexual contact. This can be avoided simply by not engaging in sexual contact when presenting open, bleeding wounds.
Other STIs, even viral infections, can be prevented with the use of latex, polyurethane or polyisoprene condoms as a barrier. Some microorganisms and viruses are small enough to pass through the pores in natural skin condoms, but are still too large to pass through latex or synthetic condoms.
Proper male condom usage entails:
- Not putting the condom on too tight at the end, and leaving 1.5 cm (3/4 inch) room at the tip for ejaculation. Putting the condom on snug can and often does lead to failure.
- Wearing a condom too loose can defeat the barrier.
- Avoiding inverting or spilling a condom once worn, whether it has ejaculate in it or not.
- If a user attempts to unroll the condom, but realizes they have it on the wrong side, then this condom should be discarded.
- Being careful with the condom if handling it with long nails.
- Avoiding the use of oil-based lubricants (or anything with oil in it) with latex condoms, as oil can eat holes into them.
- Using flavored condoms for oral sex only, as the sugar in the flavoring can lead to yeast infections if used to penetrate.
In order to best protect oneself and the partner from STIs, the old condom and its contents should be assumed to be infectious. Therefore, the old condom must be properly disposed of. A new condom should be used for each act of intercourse, as multiple usage increases the chance of breakage, defeating the effectiveness as a barrier.
Nonoxynol-9
Researchers had hoped that nonoxynol-9, a vaginal microbicide would help decrease STI risk. Trials, however, have found it ineffective[69] and it may put women at a higher risk of HIV infection.[70]
Screening
Sexually active women under the age of 25 and those over 25 with risk should be screened for chlamydia and gonorrhea yearly.[71] After being treated for gonorrhea all people should be re tested for the disease after three months.[71]
Nucleic acid amplification tests are the recommended method of diagnosis for gonorrhea and chlamydia.[72] This can be done on either urine in both men and women, vaginal or cervical swabs in women, or urethral swabs in men.[72]
Diagnosis
Testing may be for a single infection, or consist of a number of tests for a range of STIs, including tests for syphilis, trichomonas, gonorrhea, chlamydia, herpes,hepatitis and HIV. No procedure tests for all infectious agents.
STI tests may be used for a number of reasons:
- as a diagnostic test to determine the cause of symptoms or illness
- as a screening test to detect asymptomatic or presymptomatic infections
- as a check that prospective sexual partners are free of disease before they engage in sex without safer sex precautions (for example, when starting a long term mutually monogamous sexual relationship, in fluid bonding, or for procreation).
- as a check prior to or during pregnancy, to prevent harm to the baby
- as a check after birth, to check that the baby has not caught an STI from the mother
- to prevent the use of infected donated blood or organs
- as part of the process of contact tracing from a known infected individual
- as part of mass epidemiological surveillance
Early identification and treatment results in less chance to spread disease, and for some conditions may improve the outcomes of treatment. There is often a window period after initial infection during which an STI test will be negative. During this period, the infection may be transmissible. The duration of this period varies depending on the infection and the test. Diagnosis may also be delayed by reluctance of the infected person to seek a medical professional. One report indicated that people turn to the Internet rather than to a medical professional for information on STIs to a higher degree than for other sexual problems.[73]
Management
High-risk exposure such as that which occurs in rape cases may be treated preventatively using antibiotic combinations such as azithromycin, cefixime, and metronidazole.
An option for treating partners of patients (index cases) diagnosed with chlamydia or gonorrhea is patient-delivered partner therapy, which is the clinical practice of treating the sex partners of index cases by providing prescriptions or medications to the patient to take to his/her partner without the health care provider first examining the partner.[74]